In 2019 NYS Controller published an audit report of claims for Medicaid Members that impoperly received payment for SD/ER related drugs,treatment and supplies.
Please click here to read the full info.
This is a reminder for any provider that physician administered drugs and prescription for SD/ED is not covered.*
*Exception: some of the medications- that are used for ED/SD AND also have other FDA approved uses maybe covered and require an auth- both physician administered and inpatient use.
Inpatient use: alprostadil and papaverine may be covered for the treatment of a condition other than sexual or erectile dysfunction for which the drugs have been approved by the Food and Drug Administration (FDA)
Physician administered: clostridium histolyticum and phentolamine mesylate may be covered for the treatment of a condition, other than sexual or erectile dysfunction, for which the drug has been approved by the FDA and prior approval has been received.
SD- sexual dysfunction
ED- erectile dysfunction
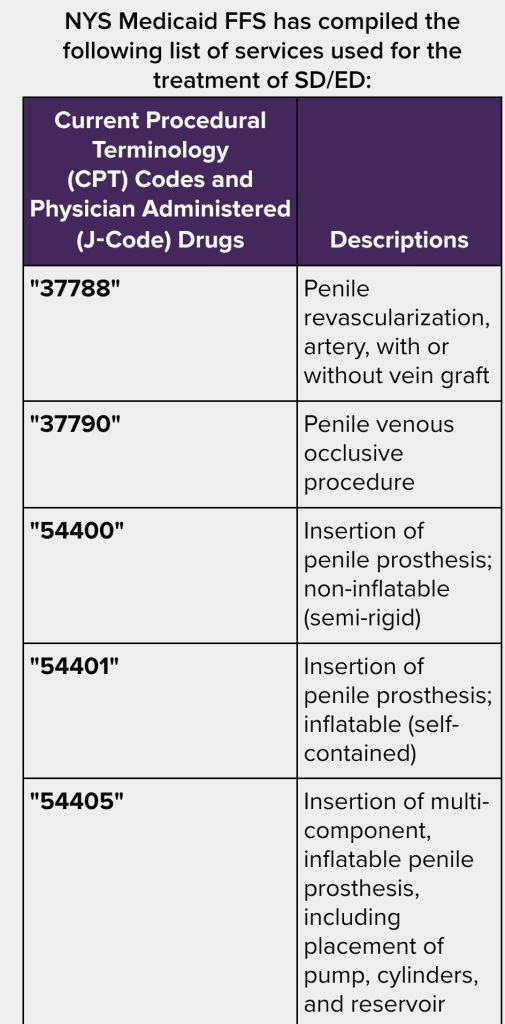
Above list is not all inclusive. For the complete list of procedures, drugs and supplies including Inpatient DX list please click here.
There are specific guidelines that NYS Fee for service and MCO plans need to follow. For the info please click here.
Find this information useful? Follow my blog for more payer updates.

Leave a comment