According to EmblemHealth-for self funded plans: Local 389 Health and Welfare fund- for the DOS 9/1/23 and thereafter have a new timely filling date for submitting claims. The new date is 90 days after the services were rendered.
This new time frame applies to In network and Out of Network providers.
Types of claims: professional, facility and other provider types
Please note that this change DOES NOT APPLY to the other ASOs (Administrative Service Organizations).
The following is still in affect:
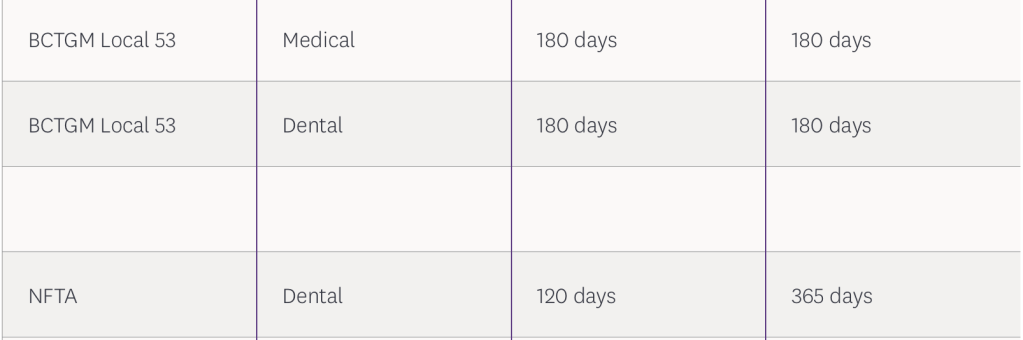
Find this blog post useful? Then follow my blog for more medical billing and coding guideline updates and changes.
In a meantime check out my other blog posts:
Previous Blog Posts:
NC Medicaid: BH community Health providers reminder
The compliance of your office is key to less audits and less disruptions to your cashflow! If you are a new provider that is submitting an application to NC Medicaid or re-enrolling, or verifying your status as a NC Medicaid Community Behavioral Health provider with NC Medicaid? Then this blog post is for you! This…
UHC Medicare Plans: oncology prior auth requirenment
Are you a provider that accepts UHC Medicare Advantage Plan or UHC Nursing Home Plan- then this blog post is for you! To prevent any disruption to your practice cash flow please be advised that for outpatient chemotherapy services above UHC members will require an auth effective DOS 6/1/26. How to request an auth? Which criteria…
Cigna- EDI clearing house requirenment
For any eligibility request done through the EDI clearing house and sent to CignaHealthcare® providers need the following information: PROVIDER NPI When is the change became effective? What does your office need to do? Find this type of content useful? Follow my blog!

Leave a comment