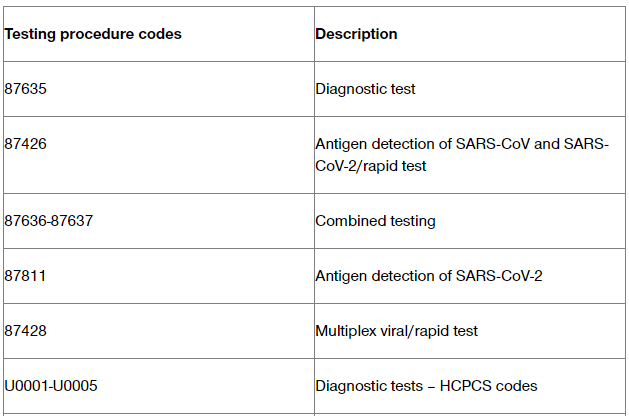
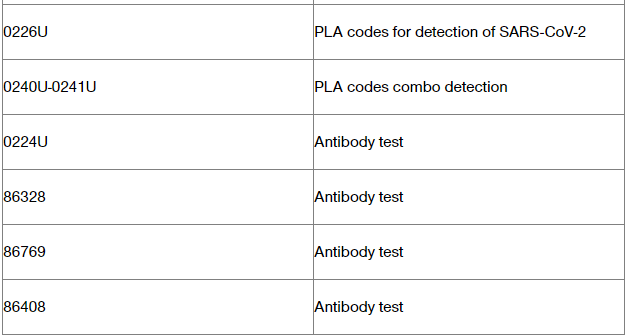
This blog post applies to genetic/molecular testing penalty waiver, that was available to providers/labs while UHC was transitioning to a new Prior Authorization and notification Platform, in 2021.
This process finished and as of Jan 1,2022 the waiver has expired!
In order to get paid for genetic/molecular testing, providers must request a prior authorization and/or an advanced notification, for any code that requires it.
Where to request prior auth/advanced notification?
Providers must go to Prior Authorization and Notification platform or by call 877-303-7736.
Performing laboratories can submit advance notifications.
If a test requires prior authorization with clinical criteria, the request must be submitted by the ordering provider.
For the current list of genetic and molecular tests that require prior authorization/advance notification, please go to UHCprovider.com/paan > Advance Notification and Plan Requirement Resources.
Questions?
For more information about the genetic and molecular lab testing prior authorization/advance notification program, please visit the UnitedHealthcare genetic and molecular testing prior authorization/advance notification (PAAN) web page and review the genetic and molecular lab testing PAAN FAQs.
Prior authorization/advance notification training
UnitedHealthcare is offering live training sessions for the genetic and molecular testing prior authorization/advance notification (PAAN) program. To register for training, please visit the UnitedHealthcare genetic and molecular testing prior authorization/advance notification (PAAN) web page.
Find this blog post useful? Follow my blog for more insurance payer updates, medical billing and medical coding guideline changes, reimbursement/medical policy updates, and more!
Recent Blog Posts: